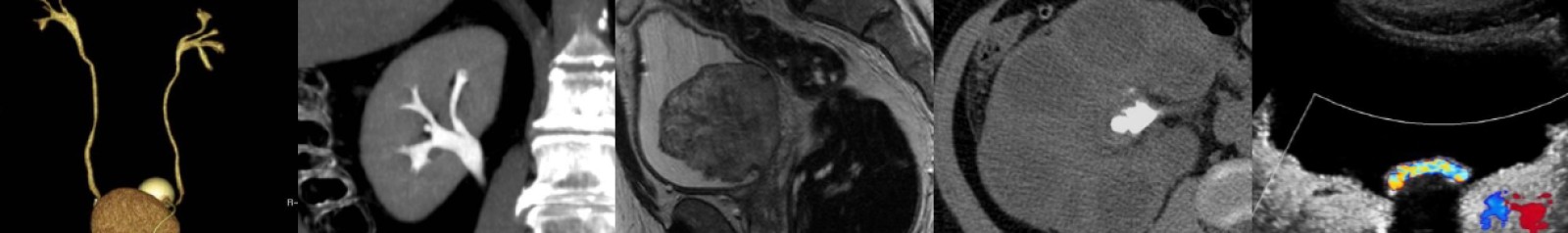
Ultrasound of Endometrioma
In this radiology lecture, we review the ultrasound appearance of endometrioma through three unique cases, including an MRI example.
Key teaching points include:
- Endometriosis = Ectopic endometrial glands and stroma outside of the uterine cavity. Includes endometriomas, extraovarian implants and adhesions.
- Endometriomas = Endometriotic cysts within ovary.
- Endometriosis is seen in about 10% of women of reproductive age.
- Presentation: Pelvic pain, dysmenorrhea, dyspareunia, infertility.
- Ultrasound: Diffuse, homogeneous low-level echoes (most specific feature) yielding a ground glass appearance. May have posterior acoustic enhancement.
- Endometriomas may have peripheral punctate echogenic foci. These foci have no internal vascular flow but can see twinkle artifact.
- Vascular flow may be present in endometrioma septations.
- Endometrioma vs. hemorrhagic cyst: Hemorrhagic cysts are acute, usually solitary and unilocular, whereas endometriomas are chronic, sometimes multiple and multilocular.
- Endometriomas can rarely (1%) undergo malignant transformation into endometrioid carcinoma or clear cell carcinoma.
- MR is the most specific imaging modality for diagnosis of endometrioma = Specificity 98%.*
- Homogeneous, T1 “light bulb” bright, T2 dark = “T2 shading.”
- Surgical treatment: Depends on disease severity from laparoscopic cyst aspiration/cystectomy to hysterectomy/oophorectomy.
- Medical management may be attempted: Oral contraceptives, GnRH agonists
*Reference: Togashi K, Nishimura K, Kimura I, et al. Endometrial cysts: Diagnosis with MR imaging. Radiology. 1991;180:73-78.
To learn more about the Samsung RS85 Prestige ultrasound system, please visit: https://www.bostonimaging.com/rs85-prestige-ultrasound-system-4
Click the YouTube Community tab or follow on social media for bonus teaching material posted throughout the week!
Instagram: https://www.instagram.com/radiologistHQ/
Facebook: https://www.facebook.com/radiologistHeadQuarters/
Twitter: https://twitter.com/radiologistHQ
Podcast: Play in new window | Download
Subscribe: Email