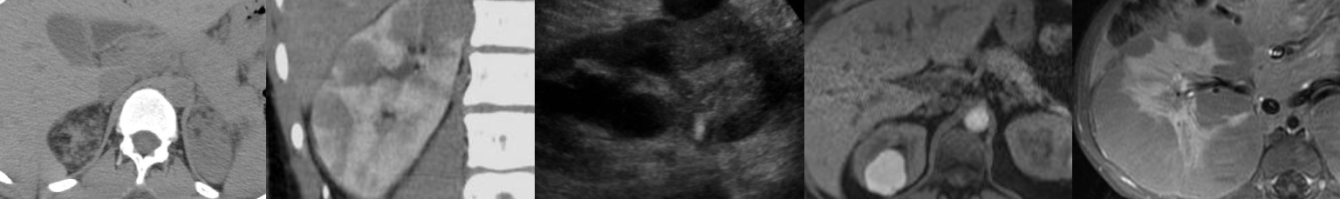
Contrast-Enhanced Ultrasound of Hemangioma
In this radiology lecture, we review the contrast-enhanced ultrasound appearance of hepatic hemangioma!
Key teaching points include:
- Microbubble contrast agents are gas-filled microspheres with a lipid or protein shell
- Sulfur hexafluoride lipid-type A microspheres: Inert gas of six fluoride atoms bound to one sulfur atom, surrounded by a phospholipid shell
- Similar in size to red blood cells, unique when compared to the molecular sizes of CT and MR imaging contrast agents. Small enough to cross capillary beds, too large to enter interstitial space = Pure intravascular agents, ideal for assessing vascularity and perfusion
- After IV injection, US contrast agents half-life is about 10 minutes (eliminated via lungs). Multiple injections possible in a single session
- Contrast-enhanced US (CEUS) has high contrast resolution: Can visualize individual microbubbles and depict a minute amount of flow = Differentiate avascular debris from small solid nodules in complex cysts. Negative predictive value of CEUS in excluding the presence of flow in a lesion is close to 100%
- CEUS also has high temporal resolution: Effectively eliminates motion artifact, a major source of artifact on CT and especially MRI scans. In elderly or debilitated patients, or when there is any other cause of motion, CEUS may be the contrast-enhanced modality of choice
- Accuracy and specificity of CEUS for the diagnosis of hepatic hemangioma approaches 100%
- Mechanical index (MI) = Measure of acoustic power output. At high MI, microbubbles burst. At low MI, microbubbles are preserved and have a nonlinear response to US, unlike other tissues which have a linear response. Allows for creation of a vascular-only image
- Hemangioma has peripheral discontinuous globular enhancement in arterial phase. Progressive centripetal contrast filling and iso- or hyperenhancement in portal venous and late phase
- Non-hepatocellular malignancy typically demonstrates early (less than 1 minute) and/or marked washout
- Hemangioma filling may be partial or complete depending on lesion size
To learn more about the Samsung RS85 Prestige ultrasound system, please visit: https://www.bostonimaging.com/rs85-prestige-ultrasound-system-4
See more impressive visuals by filmmaker and freelance motion graphics artist Nick Shaheen: https://www.instagram.com/nickhshaheen
Click the YouTube Community tab or follow on social media for bonus teaching material posted throughout the week!
Spotify: https://spoti.fi/462r0F2
Instagram: https://www.instagram.com/Radquarters/
Facebook: https://www.facebook.com/Radquarters/
X (Twitter): https://twitter.com/Radquarters
Reddit: https://www.reddit.com/user/radiologistHQ/
Podcast: Play in new window | Download
Subscribe: Email